How it Works
It’s all about the data.
Lab testing provides the data you need to build and maintain a care plan that is as custom and convenient as possible. Read over 400 expert-reviewed lab test guides to better understand what each test measures, how it’s used, when you might need a particular test, and more.
View Testing Guides
Turn information into action.
If you need a test, order lab tests and at-home test kits through our laboratory partners directly. We partner with certified labs to give you the most reliable and secure experience possible.

Make informed health care decisions
Most results are ready 1-2 days after samples are received at the laboratory. Your results will be accessible through the partnering laboratory or company that your order is processed through.
View ResourcesFeatured Test Guides

Thyroid Function Testing

Blood Testing
Medical Review Board
Resources

How to Select an At-Home STD Test
Learn more about at-home STD tests, such as what they measure, their benefits and drawbacks, as well as our top picks for 2022.
Learn More
How to Select an At-Home Sleep Apnea Test
Learn more about at-home sleep apnea tests, such as what they measure, their benefits and possible downsides, as well as our top pick for 2022.
Learn More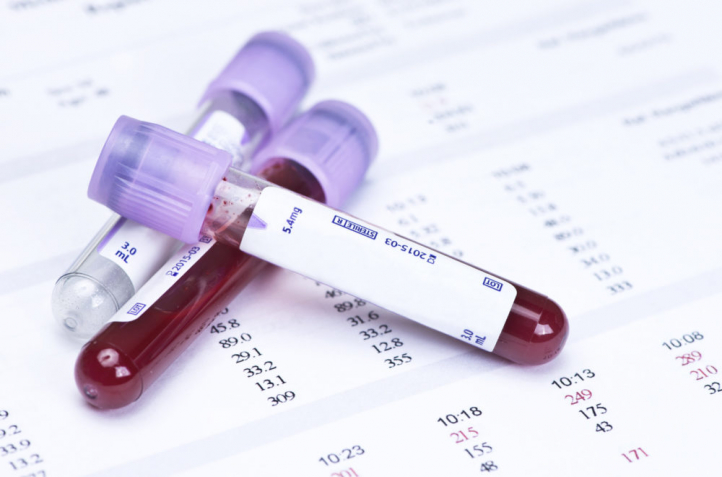
Reference Ranges and What They Mean
A reference range is a set of values that includes upper and lower limits of a lab test based on a group of otherwise healthy people. By comparing your test results with reference values, you and your health care provider can see if any of your test results fall outside the range of expected values and gain clues to help identify possible conditions or diseases.
Learn MoreLatest News
Antibiotic-Resistant Bacteria Cause More Deaths than HIV or Malaria
A new global report found that more people died of infections caused by antibiotic-resistant bacteria than HIV or malaria in 2019. Bacterial infections that don’t respond to antibiotic treatment are a serious public health threat. Misuse and overuse of antibiotics have contributed to this increasing worldwide problem.
Antibiotic resistance is when bacteria are able to survive and grow in the presence of one or more antibiotics.
Learn More
















